Light sheet microscopy
Light sheet fluorescence microscopy (LSFM), in contrast to epifluorescence microscopy, only uses a thin slice of illuminated sample that is perpendicular to the direction of observation.

Small Animal Imaging
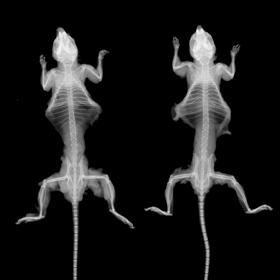
Luminescence emissions from reporter genes provide a quantitative model for studying the development of human diseases. As the amount of light collected using this method is very little, an ultra-sensitive camera is required to record luminescence emissions as they propagate through soft tissues.

Contact Us
22 Theaklen Drive,
Saint Leonards-on-sea,
TN38 9AZ,
United Kingdom
Phone:
+44 (0)1424 444883
💬



